The pressure on women to have the ‘perfect’ birth
Many women strive for a “beautiful” birth experience without medical intervention. It works for some women, yet this ideal can be damaging if plans don’t materialise.
Warning: This story includes details of traumatic birth that some readers may find distressing
When Emma Carr fell pregnant in 2021, she had a vision for her ideal birth. At the most basic level, she wanted to feel empowered, listened to and in control. But, like many women, Carr’s vision went further than that. In particular, she hoped for a ‘natural birth’ – generally described as a vaginal delivery with as little medical intervention and pharmacological pain relief as possible.
She followed two courses, including one popular approach known as ‘hypnobirthing’, which taught relaxation and breathing to help ease pain and help stay present during delivery. And, as her instructors recommended, she watched videos of healthy, happy, non-traumatic births to get her into the right mindset.
“You watch all these videos of these babies being born, and it’s so beautiful,” says Carr, 36, who lives in London. “They come out really easily, and the woman grabs them, and you’re just like, ‘That’s what’ll happen to me’.”
But when Carr’s water broke, the fluid contained meconium – the foetus’ stool, which can be dangerous for mother and child. After she rushed to hospital, doctors told her they had to get the baby out immediately. Two hours later, she lay on the operating table under bright lights. Far from her ideal, intervention-free vaginal birth, her baby was born by caesarean section. Worst of all, she says, was how unprepared she felt for this kind of outcome, given how focused she had been – and had been encouraged to be in the courses she followed – on creating a positive mindset.
“If I hadn’t had in my head how it ‘should’ have gone, then I wouldn’t feel like it was a failure,” she says. “I just wish [my instructors] were a bit more open about how these births happen. That it doesn’t always go right, just because you did hypnobirthing.”
While she was pregnant, Carr says friends tried to warn her she might not have the labour she was hoping for. But she dismissed them, thinking they probably hadn’t gone in with the mindset or techniques she would.
“People that you would normally listen to, you stop listening to, because you’ve got these other people in your head telling you birth should be natural and magical, and that your body is just perfectly designed to do it,” she says. “But I don’t think mine was.”
Many women do benefit from this approach to birth. Some even experience the ideal scenario that they hoped for. With the right techniques – like breathing, listening to affirmations or massage – some advocates say birth can be enjoyable, even orgasmic. But others, like Carr, are left reeling, and not only from a traumatic birth – they feel as if having been fixated on that vision, and not preparing for the many ways in which it might not happen, made their experience even worse.
Birth of a movement
For much of history, women frequently died in labour – as often as in one in every 100 births in the 1600s and 1700s. Scientific advances including antibiotics mean that the maternal mortality rate has plummeted. As the medical community expanded its focus beyond safety, narcotic pain reduction techniques like the epidural became common in many countries. Even today, maternal mortality is highest in countries where there might not be adequate medical care for complications more easily treated elsewhere.
After preparing themselves for an ‘ideal’ birth experiences, some women feel as if they’ve failed if they end up having medical intervention, like C-section (Credit: Getty Images)
Many birthing parents choose modern pain-management as the right choice for them, and many doctors also recommend it. But other women and health practitioners believe the birthing process has gone too far in this direction, saying that an over-reliance on medical interventions can be unnecessary, risky, even dehumanising. In the 1960s, for example, women in wealthy countries often gave birth while sedated with general anaesthesia. They may not have felt pain, but they couldn’t feel present or make in-the-moment decisions regarding their care, either.
Today, many women now strive for – and idealise – what is often referred to as a ‘positive birth’. Coined by UK birth campaigner and Positive Birth Movement founder Milli Hill, the term ‘positive birth’ wasn’t, originally, meant to describe any particular kind of labour. It has broadened.
“A positive birth does not have to be ‘natural’ or ‘drug free’ – it simply has to be informed from a place of positivity as opposed to fear,” the association’s website reads. “You can birth with positivity in hospital or at home, with or without medical intervention.” Rather, the website outlines, it is an experience where a woman feels she has “freedom of choice, access to accurate information, and that she is in control, powerful and respected” as well as one that she “goes on to enjoy, and later remember with warmth and pride”.
Still, many women who follow positive birth courses say they feel an undercurrent of idealising ‘natural’ births in particular. For some instructors, a big part in emphasising how birth can be ‘positive’ comes with talking about how a woman’s body is ‘designed’ to give birth – and the subtext can be that medical interventions impede, rather than assist, this process.
A main tenet of many of these approaches, for example, is that fear and anxiety increase the body’s production of hormones like adrenaline, which can slow down labour and make contractions feel worse. With techniques including making one’s birth space feel homey and comfortable; being supported by a birth partner (or team); using breathing or meditation techniques; and, above all, going into labour feeling relaxed and confident, the idea is that you can encourage the production of oxytocin instead, making labour faster and less painful.
The popularisation of ‘natural’ birth in particular has a long history: it dates back to at least the 1930s, interestingly around the same time that the first college of obstetrics and gynaecology was founded. And for many women, approaches like these have never held much weight: if you want to give birth as painlessly as possible, why not just use every modern medical intervention and drug available?
But for others, this image of the ‘natural’ ideal birth has stuck, amplified by a booming birth-education industry. On social media, beautiful stories of relaxed water births with soothing music and candles everywhere abound.
If I hadn’t had in my head how it ‘should’ have gone, then I wouldn’t feel like it was a failure – Emma Carr
There are many benefits to these birth movements, not least their aims to put the decision-making back into the birthing parent’s hands. But with both ‘positive’ and ‘natural’ increasing as common cultural ideals, for some women, there is a downside. No number of classes or relaxation techniques can always overcome the reality that the circumstances of every birth are different; that there are huge racial and ethnic disparities in quality of care; that maternity care can be subpar overall; or that women sometimes feel pressured to accept interventions. Even the simplest goals of feeling empowered during labour, or having fond memories of birth, can feel out of reach. (It’s also worth noting that both the time and financial investment that some of these courses require make them out of reach for many – they can cost less than $50 (£41) online or upwards of $1,000 [£815] for private guidance, and usually require at least several hours of instruction).
Proponents of this approach say that medical providers need to step up to fix these problems, rather than mothers lowering their expectations. But in the meantime, for women whose labours don’t go as planned, having a highly specific – and often idealised – birth vision in mind can put undue pressure on what is, ultimately, an unpredictable experience. In the worst case, they can feel as if they have failed themselves – or their babies.
An ideal – not a norm
The ‘natural’ birth, in which everything unfolds perfectly and without a need for intervention, remains far from the norm. In the US in 2020, for example, CDC data shows nearly a third of all births included an induction of labour. In addition, a third were caesarean deliveries (C-sections). Home births, often held up as the ultimate ‘natural’ labour, accounted for just 1% of all births.
But for many birthing parents who emphasise natural birth as the goal of their ‘positive’ approach, their labours don’t always go to plan – and this can have ripple effects. Some mothers say that, by focusing only on their ideal birth, they were blindsided by the reality – and felt additional grief for not getting to experience the perfect birth they wanted. In one study, 15% of women who had an unplanned C-section reported that they felt as though they’d “failed”.
Edwina Moorhouse considers herself a ‘positive’ birth convert after smooth birth experiences with all three of her children (Credit: Courtesy of Edwina Moorhouse)
FAMILY TREE
This article is part of the BBC’s Family Tree series. Explore more from Amanda Ruggeri, including in-depth looks at motherhood ambivalence and why new mums are expected to ‘bounce back’ quickly.
In Toronto, Andie Perris, 38, wanted “as much of a natural experience as possible” before her first birth. She took a hypnobirthing course, listened to relaxation audio tracks and read Ina May Gaskin’s On Childbirth, which was “full of stories of serene deliveries of women breathing down their babies and their body taking over”, she says.
“I had seen and heard of these beautiful birth stories, and that’s what I was expecting for myself because I had done all the work,” she says. “I really believed that it would change the outcome of my delivery.” Instead, Perris was in labour for almost 24 hours. Her pelvic floor was “completely destroyed”. Her son, who wasn’t descending properly, was ultimately delivered by vacuum. Perris had a postpartum haemorrhage.
Looking back, she says, she probably should have had a C-section. But she had been set against it. “Feeling like there was one ‘right’ way to have a baby, it made me laser focused on that right way,” she says. “And of course, there’s not one right way. But I was so wrapped up in this vision of how nature ‘intended’ you to have a baby.”
Because she was so focused on maintaining a positive mindset going into her labour, Perris says, she didn’t prepare herself for the possibility that it might go differently. As a result, “when things started to go sideways, it was very hard for me to adapt”.
For her second child, she tried to listen to the same relaxation audio tracks she’d used to prepare for her first. She found it so anxiety inducing that she had to stop.
Emiliana Hall is a UK-based doula and founder of The Mindful Birth Group, which helps women prepare for birth. Hall, who says her approach eschews idealising any form of labour and instead covers all potential outcomes, reports she is now seeing a wave of second-time mothers saying that, after doing a ‘positive’ birth approach, their first experience didn’t go as they thought.
The problem, says Hall, isn’t just that they had a negative experience. It’s that they blame themselves for it. This can be the risk of an approach that focuses so much on mindset, she says: many courses recommend listening only to positive birth stories, or even replacing negative words like “contractions” with “surges”, to keep fear and anxiety, and therefore stress hormones and, theoretically, pain, at bay. If a woman does wind up feeling pain or trauma, she might question if it was because she wasn’t relaxed enough.
“When it doesn’t work, it feels like either they failed, or it was a complete waste of time,” says Hall. “But there are so many things that you can’t control.” In her courses, says Hall, she is careful not to even use the phrase “positive birth” – because despite teaching techniques to make birth better, she’s acutely aware that there’s no guarantee things will go as planned.
‘I can’t just have been lucky three times, right?’
Of course, plenty of mothers have found positive birth approaches helpful, even transformative.
In Berlin, Edwina Moorhouse, 32, thought they sounded “hippie”. But after watching a YouTube vlogger enthuse about her experience, she put aside her scepticism. “I really wanted that joy that you see that she has,” she says. She took a hypnobirthing course, practised breathing techniques and underwent weekly acupuncture. She had a smooth, fast water birth. Her second labour was similar. By her third child, where she dragged pink Himalayan salt lamps, big headphones and warm socks to her hospital room to make it cosier, she was a convert.
There’s not one right way. But I was so wrapped up in this vision of how nature ‘intended’ you to have a baby – Andie Perris
“I can’t just have been lucky three times, right? There must be something to this,” she says. “To think that by my third son, I was religiously listening to hypnobirthing mp3s, flooding my brain with positive stories on YouTube, spending a stupid amount of money on this one shampoo that had a scent that offered instant pain relief – I am completely unrecognisable to the woman that was pregnant six years ago.”
Indeed, there is some evidence that the techniques taught in many of these birth courses can reduce pain and epidural use, lessen the number of interventions and the length of labour itself, lower C-section rates, and improve a mother’s overall birth experience. But these findings aren’t always replicated, and some aspects seem to be more useful than others. One large review showed although some popular elements, like the presence of a trained birth partner or using music or massage to relax, helped reduce the likelihood that a woman would look back on her birth experience as “negative”, other techniques were less useful.
Another review showed music, yoga and relaxation techniques like guided meditations might help reduce pain. But they made no difference in lowering the rates of birth interventions including C-sections, or of whether women ultimately needed pharmacological pain relief.
From a medical standpoint, it’s generally accepted that, since each intervention has its own risks and costs, they shouldn’t be done unnecessarily or, in the case of pain-management interventions, without full, informed consent. An epidural, for example, may be linked to a longer second stage of labour and higher chance of needing an instrumental birth and, in rare cases, fever or nerve damage. But women who follow ‘positive’ birth approaches say that the undertone sometimes can go further than that, making birthing parents feel as if any intervention is “bad”.
“The message is that you’re made for it, it’s natural, women have been doing it since the dawn of time, your body knows what it’s doing, your baby knows what it’s doing,” says Beth Sandland, a lifestyle blogger and founder of the digital magazine The Motherhood Edit. “I wouldn’t say it’s fear mongering. But I would say that there is definitely an undertone of, ‘the hospitals don’t necessarily act in your best interest. The doctors don’t necessarily have a realistic approach to physiological birth'” in some of the courses and social-media accounts that she’s seen, says the 26-year-old.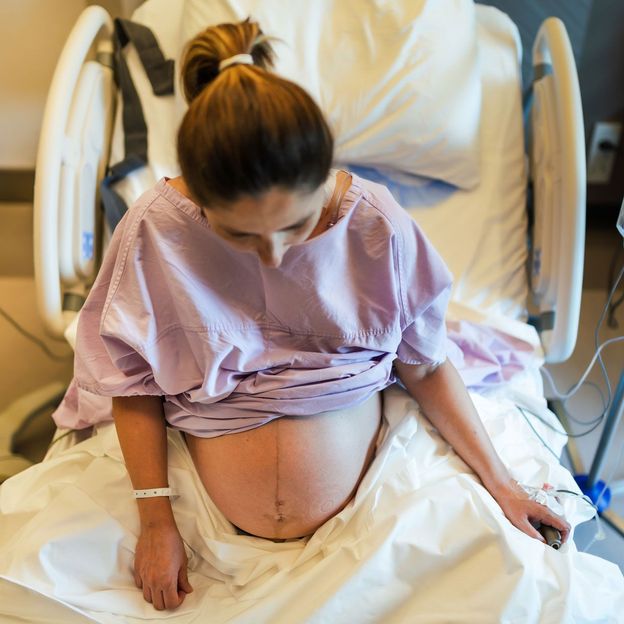
For many, the most important aspect of having a ‘positive’ birth comes down to one thing: autonomy (Credit: Getty Images)
Yet interventions alone aren’t necessarily the ultimate arbiter of a ‘positive’ experience. Indeed, research has found that one of the most important aspects of whether a woman thought her birth was positive was how long the labour took. Those who had shorter labours were more satisfied – even when their labour was shortened by an intervention like, say, oxytocin augmentation. Given the effect of prolonged labour, the researchers concluded, “interventions to avoid that could result in a ‘net benefit'”.
For many women, of course, interventions also can be lifesaving. “How it’s presented is like, you don’t have to do what they tell you. And like the doctors are kind of out to get you, in a way,” says Carr. “They’re like, ‘Oh, it’s not risky. It’s natural.’ That can be true, but not always. I think for me, there was risk. If I hadn’t had any medical intervention, one of us might not have survived … I don’t think in the wild I would have birthed that baby easily.”
‘I studied for it like it was an exam’
A big part of the positive birth movement involves empowerment. Indeed, feeling in control and being involved in decision-making is a big part of having had a positive experience. And even if there are complications during delivery, some women still find certain techniques that help them feel in control to be useful.
In Glasgow, Anna Murray, 34, did all of the preparation she possibly could for her labour. “I studied for it like it was an exam,” she says. She did a private course with a doula, read books, followed a yoga hypnobirthing course. She even had a Google Drive folder with all of her audio tracks and yoga videos for different birth positions.
In the end, she needed an unexpected caesarean – her son had grown too big and was in a fixed position that no amount of exercises could turn. But the breathing techniques helped her stay calm on the operating table, she says. “It can help you have a calm controlled birth whatever you have. But ultimately, it can’t really give you any more control over what’s going to happen,” she says.
Murray’s birth speaks to the nuanced nature of how many women experience the positive birth ideal today. For some, it pans out exactly as they dreamed, and gives them the techniques to help make it happen. For others, it’s a crushing disappointment. And for those like Murray, the techniques can provide useful tools to make the best out of a difficult situation.
Ultimately, for many, the most important aspect of having a positive birth comes down to one thing: autonomy. That doesn’t just mean feeling empowered, whether in a labour ward or at a home birth. It also means not feeling pressured to birth in any specific way.
And, as a culture, it means recognising that every woman’s physiology, medical conditions and birth process will look different, being careful not to lionise any particular kind of experience as a cookie-cutter ideal – whether it’s one that takes place under anaesthesia or in a candlelit bath.























Hi, this is a comment.
To get started with moderating, editing, and deleting comments, please visit the Comments screen in the dashboard.